If you know anything about medicine or have older relatives, you’ll have heard about at least one person using statins.
And it’s not hard to see why, given how insanely popular and profitable these cholesterol-lowering drugs are:
“Since their introduction in the late 1980s, statins have been a particularly lucrative class of drugs, primarily for pharmaceutical giants Pfizer, Merck Sharp & Dohme and AstraZeneca.
Pfizer’s Lipitor is the most profitable drug in the history of medicine. At its peak in 2006, yearly revenue for Lipitor exceeded $12 billion USD.
Despite their patents recently expiring, revenue for statins is still expected to rise, with total sales on track to reach an estimated $1 trillion USD by 2020. Statins are very big business.”
But what is the REAL truth on statins?
Are these drugs the miracle medical solutions many doctors say they are?
Or is there a bigger cover-up going on – one where ineffective drugs are being promoted in order to put more money in Big Pharma’s pockets?
These questions and many more will be answered in this article.
But first, it is imperative to understand how cholesterol works in our body, followed by a clear picture of the mechanism through which statins “treat” people.
MANY thanks to Dr. Rob Kominiarek of RenueHealth.com and Dr. Kenneth Wilgers for their comments and insights that contributed to the research and writing of this article.
Table of Contents
ToggleWhat Is Cholesterol And What Does It Do?
Cholesterol is a steroid molecule which is found in every single cell in your body as a vital structural component of the cell’s membrane.
It is produced in your nerve tissue, liver, brain tissue and your bloodstream.
In addition to helping with digestion, cholesterol is also a very important precursor of several important hormones:
- Vitamin D
- Testosterone
- Glucocotricoids (for generating glucose)
- Estrogen
- Bile salts (not a hormone but they do help break down fats found in food)
And as any diet fanatic would know, cholesterol is found in everyday foods such as cheese, meat, and egg yolks.
There are generally two types of cholesterol you need to monitor for your health.
Low-Density Lipoproteins (LDL) – The “Bad” Cholesterol
LDL cholesterol is perceived to be “bad” because too much leads to fatty buildup in your arteries, which harden over time and become plaques.
This leads to the arteries becoming narrower and therefore blood flow is restricted (i.e. atherosclerosis).
If this goes on for too long, you leave yourself at greater risk for cardiovascular diseases such as stroke, peripheral artery disease, chest pain (angina) and a potential heart attack.
High-Density Lipoproteins (HDL) – The “Good” Cholesterol
HDL cholesterol is known as the “good” cholesterol because it transports cholesterol from your body to your liver.
While HDL can carry LDL away from the arteries to be broken down, it only carries 25-33% of blood cholesterol.
From here, the takeaway conclusion seems simple:
Elevate your HDL levels while lowering your LDL levels and you’ll be just fine.
So where do statins come into the picture?
An Overview Of Statins: Why Are They Prescribed So Often?
Statins are prescription drugs that have two primary functions:
- Stop production of cholesterol by blocking HMG-CoA reductase (the enzyme in your liver that produces cholesterol.
- Reabsorb existing cholesterol that built up as plaques in your artery walls (in the form of LDL) so it can perform essential bodily functions.
There are numerous statins currently available in the United States market, such as the following:
- Pitavastatin (Livalo)
- Rosuvastatin (Crestor)
- Simvastatin (Zocor)
- Pravastatin (Pravachol)
- Lovastatin (Altoprev)
- Atorvastatin (Lipitor)
A quick look in the scientific literature will find several purported health benefits of statins.
They include reducing the risk of cardiovascular disease and neurocognitive disease, lowering inflammation, and much more.
To date, here’s what we know about statin usage across the country:
- Roughly 35 million Americans are using statins
- 17% of adults between 40-59 use statins, and that number jumps up to 48% for adults older than 75 years old.
- Amongst adults aged 40-64, those who have health insurance are far more likely to be on a statin
Statins are commonly prescribed following a cardiovascular event such as a heart attack, and/or if lifestyle stages have failed to lower your cholesterol.
Should Doctors Be Attempting To Lower Cholesterol?
Here’s the problem we run into: There is no definitive cause-effect relationship established between cholesterol and heart disease, only an association.
An association which may not stand on solid scientific ground.
It turns out the connection is weak at best and more likely nonexistent, according to a comprehensive review of literature studies done in 2018:
“The hypothesis that high TC (total cholesterol) or LDL-C (low-density lipoprotein cholesterol) causes atherosclerosis and CVD has been shown to be false by numerous observations and experiments.”
“The fact that high LDL-C is beneficial in terms of overall lifespan has been ignored by researchers who support the lipid hypothesis.”
“That high LDL-C is the cause of CVD (cardiovascular disease) in FH (familial hypercholesterolemia) is questionable because LDL-C does not differ between untreated FH individuals with and without CVD.”
“Our search for falsifications of the cholesterol hypothesis confirms that it is unable to satisfy any of the Bradford Hill criteria for causality and that the conclusions of the authors of the three reviews are based on misleading statistics, exclusion of unsuccessful trials and by ignoring numerous contradictory observations.”
In simpler terms, artificially lowering cholesterol numbers is not effective for reducing cardiovascular risk in patients.
And it’s not so much that a high total cholesterol (TC) number is bad, but how high it is relative to HDL:
“A high TC to high-density lipoprotein (HDL) ratio is the best predictor of cardiovascular risk (hence this calculation, not LDL, is used in recognised cardiovascular risk calculators such as that from Framingham).
A high TC to HDL ratio is also a surrogate marker for insulin resistance (ie, chronically elevated serum insulin at the root of heart disease, type 2 diabetes and obesity).
…A high TC to HDL ratio drops rapidly with dietary changes such as replacing refined carbohydrates with healthy high fat foods.”
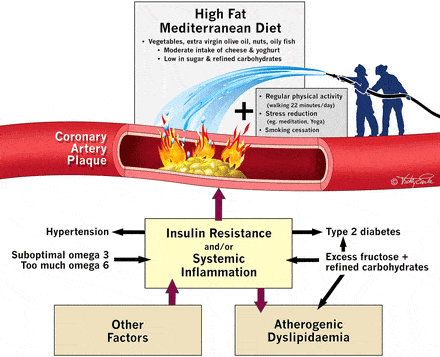
The editorial I just quoted even sums up the issue IN ITS TITLE:
“Saturated fat does not clog the arteries: coronary heart disease is a chronic inflammatory condition, the risk of which can be effectively reduced from healthy lifestyle interventions”
Furthermore, higher HDL levels will decrease your chance of cardiovascular disease:
“Since the first discovery of an inverse correlation between high-density lipoprotein-cholesterol (HDL-C) levels and coronary heart disease in the 1950s the life cycle of HDL, its role in atherosclerosis and the therapeutic modification of HDL-C levels have been major research topics.
The Framingham study and others that followed could show that HDL-C is an independent cardiovascular risk factor and that the increase of HDL-C of only 10 mg/L leads to a risk reduction of 2–3%.”
The authors of the paper I just quoted made a very important observation near the end.
Specifically, in a state of chronic inflammation, HDL particles can actually fuel the inflammatory process.
So what can we conclude from all this?
It’s very simple…
When we make healthy lifestyle choices that reduce insulin resistance and systemic inflammation, undesirable cardiovascular events happen a lot less often.

Statins Don’t Actually Help You Live Longer

But the problems with statins do not stop at heart disease.
The guidelines for prescribing statins have changed so dramatically to the point where otherwise healthy individuals are now eligible for these drugs:
“When the US National Cholesterol Education Program (NCEP) revised its definition of “high cholesterol” by dramatically lowering the threshold, it meant millions more people would become eligible for statins overnight.
The decision was not based on any new scientific data but rather the increasingly popular notion that “lower is better”.
The move sparked a furore when it was revealed that eight out of nine members on the 2004 NCEP guideline committee had direct financial ties to statin manufacturers.
Then, in 2013, the American College of Cardiologists (ACC) and the American Heart Association (AHA) changed their guidelines to reflect a person’s “calculated risk”.
Again, it meant that millions more adults would be prescribed statins, most of whom were older people without heart disease and for whom the evidence for benefit was lacking.”
This makes perfect sense considering the financial benefits doctors get out of prescribing expensive brand-name statins:
“Researchers from Brigham and Women’s Hospital and Harvard Medical School reviewed the records of about 1.6 million prescriptions for statins covered by Medicare Part D in Massachusetts in 2011.
Researchers found that physicians who didn’t receive industry money prescribed brand-name statins at a rate of almost 18 percent. Those who did take money prescribed brand-name drugs at a rate of almost 23 percent.
…Overall, researchers found that for every $1,000 spent on doctors, brand-name drug prescriptions increased 0.1 percent.”
Let’s suppose we put aside the lack of any real connection between statin use and lowered risk of heart disease.
What about survival?
Unfortunately, things don’t get any better.
Several studies such as this one (and this one) have concluded that statins are ineffective in reducing the risk of death in older individuals without any history of heart disease:
“In participants older than 74 years without type 2 diabetes, statin treatme
t was not associated with a reduction in atherosclerotic CVD or in all cause mortality, even when the incidence of atherosclerotic CVD was statistically significantly higher than the risk thresholds proposed for statin use”
The same can be said for middle-aged men:
“The Web site of the ALLHAT study says it best: “trials [primarily in middle-aged men] demonstrating a reduction in [coronary artery disease] from cholesterol lowering have not demonstrated a net reduction in all-cause mortality.”
Moreover, it appears as if lowering your intake of dietary cholesterol doesn’t do the trick either:
“Reducing cholesterol blood levels by reducing dietary saturated fats is commonly recommended, but an exhaustive review and meta-analysis of 72 dietary studies concluded that reduced consumption of saturated fat does not reduce cardiovascular mortality”
When a systematic literature review of all the studies are done, you’ll find a “surprisingly small average gain in overall survival”:
“Their literature review found that if you take a statin medication for two to six years to prevent your first heart attack—this is called primary prevention—your death will be postponed by an average of three days and five hours.
If you take a statin for two to six years after you have had a heart attack—this is called secondary prevention—your death will be postponed for just over four days.”
And what about the women?
When statins are used for primary prevention (women with no history of heart disease) or secondary prevention (women with pre-existing heart disease), no changes in the death rate are observed.
I’m not quite done yet…
A major clinical trial known as PROSPER (Pravastatin in elderly individuals at risk of vascular disease) examined seniors ages 70-82 who had a history of heart disease or possessed risk factors for it.
The study DID find a lower incidence of heart disease, but at a cost.
This decrease was almost entirely negated by a corresponding increase in cancer cell deaths – 25% more frequent in the group taking pravastatin!
As a result, overall mortality between the pravastatin and placebo groups after 3.2 years were nearly identical.
This is troubling when you consider how rapidly the rate of heart disease rises in men as they age.
According to the American Heart Association:
- 70.2% of men ages 60-79 have 1 or more types of cardiovascular disease
- This number jumps up to 83% for men who are 80 years of age or older
- For men ages 35-44, the annual rate of first-time cardiovascular events is 3 per 1000. It jumps to 74 per 1000 in men ages 85-94.
With all of the overwhelming evidence available, one might ask themselves how statins developed a stellar reputation in the first place.
How Are Statin Clinical Trials Manipulated To Present False Conclusions?
The answer as to why statins show positive results in trials involving overall survival are simple: Statistical deception.
Statins are certainly effective for reducing cholesterol levels, but they clearly do not substantially improve cardiovascular outcomes.
So how does Big Pharma deceptively create the appearance that lowering cholesterol leads to a lower incidence of heart disease?
Through a statistical calculation called “Relative risk reduction” (RRR).
The best way to show you how this is done is through an example scenario used in a groundbreaking 2015 review debunking several clinical trials involving statin use.
(BTW…credit goes entirely to the authors of the paper. I’m just simplifying what they’re saying to make it easier to understand).
Suppose you have a 5-year clinical trial which involves 2000 middle-aged men of good health.
Your main outcome is to determine if prescribing statins will prevent heart disease.
You give 1000 of the men a placebo, and a statin to the other 1000.
And let’s say we come up with the following results:
- % of placebo patients suffering from heart attack: 2%
- % of pravastatin patients suffering from heart attack: 1%
This is not a stretch, as it is typical for 2% of these men to experience a nonfatal myocardial infarction (MI) over 5 years.
1% of men in the statin group experienced a MI, while 2% of men in the placebo group had a MI.
To determine the RRR, we would divide the % of pravastatin patients by the % of placebo patients:
1% ÷ 2% = 0.5
This would represent a 50% risk reduction by the drug in the treated group.
“Look! The statins reduced the incidence of heart disease by 50%!”
Of course that’s how they would say it – nobody in their right mind would be impressed by a 1% point improvement.
But there are two indicators of clinical usefulness which prove to be superior for evaluating the effectiveness of the statin in question.
The first indicator is the “Absolute risk reduction” (ARR), which is the “absolute” risk difference in event rate between a treatment group and the control group.
You calculate it by subtracting the % of placebo patients from the % of pravastatin patients.
In this case, 2% – 1% = 1%.
This means only 1% of the patients benefit by taking the statin.
The second indicator is the “Number needed to treat” (NNT), which tells us the number of patients you need to treat with a medication in order to achieve the desired income.
We calculate the NNT by taking the inverse of the ARR:
1 ÷ 0.01 = 100.
The higher the NNT, the more ineffective the drug is.
If the NNT for preventing a heart attack is 100, it means 100 patients must be treated to prevent ONE patient from having a heart attack.
The authors say it best:
“Put another way, the chance of not suffering from an MI during the 5-year period without treatment was 98% and by taking a statin drug every day it increased by 1 percentage point to 99%.”
I strongly urge you to read the review as it debunks several clinical trials and shows you how the RRR is used in action.
In addition, investigative journalist Dr. Maryanne Demasi’s presentation on the shocking amount of statin disinformation is a MUST-SEE!
Harmful Side Effects Of Statins
I haven’t even talked about the side effects of statins yet, but we already know they are ineffective for improving survival or reducing heart disease.
Putting aside the numerous drugs statins negatively interact with, there are several harmful side effects you should know about:
- Stimulating heart failure and atherosclerosis (blockage of arteries)
- Greater risk of staph skin infections
- Lower testosterone levels
- Higher risk for new-onset diabetes
- Increased caloric and fat intake
- May trigger a rare autoimmune muscle disease
- Adverse mood and behavioral change
- Lupus-like syndrome
- Disturbed sleep patterns
I could go on forever with this list, but I believe the message is clear.
In the majority of cases, statins are not measurably improving your health.
In the worst of cases, you may be destroying your health with statins.
When Are Statins Acceptable Medical Interventions?
It is quite rare for someone to truly have a clinical need for statins.
You’re talking about very specific population groups in the 40-75 age range who are severely inflamed, such as the following:
- Their 10-year risk of cardiovascular disease exceeds 7.5%
- LDL readings are greater than 190 mg/dL
- Diabetics
- Individuals with plaque-related diseases like heart disease and stroke.
I would also like to add that Dr. Mark Gordon has successfully used statins in patients with TBI (traumatic brain injury) due to their mild anti-inflammatory effect.
As a side note, I strongly recommend you supplement with CoQ-10 if you are going to take statins.
I explain precisely why in The TOT Bible:
“Statins have been found to significantly lower Co-Q10 levels, however, so it is essential for statin users to supplement with Co-Q10 to help restore depleted levels.
Ubiquinol Kaneka QH Coenzyme Q-10 (CoQ-10) is a vitamin- like substance found throughout the body, especially in the heart, liver, kidney, and pancreas.
Coenzyme Q10 may protect against many age-related disorders including cancer, heart disease, diabetes, and various neurological disorders.
Taking 200-300 mg a day has been clinically proven to offer powerful disease-resistant benefits.”
The goal should ALWAYS be to gradually titrate off of them once lifestyle interventions are fully in place.
Natural Lifestyle Alternatives To Taking Statins

Fortunately for you, several viable alternatives exist to taking statins.
Most of these can be done for free!
Aspirin
According to a study in the British Medical Journal, aspirin is equally as effective as statins for treating heart disease in people with pre-existing heart disease.
It’s also far safer, with fewer side effects and risks.
And it’s 20 times cheaper!
Diet and Exercise
Who would possibly think the dietary recommendations given to us by health authorities would lead us towards heart disease and eventual death?
Well, apparently they do:
“The long-established dietary recommendations have created epidemics of obesity and diabetes”
“Foods loaded with sugars and simple carbohydrates, or processed with omega-6 oils for long shelf life have been the mainstay of the American diet for six decades. These foods have been slowly poisoning everyone.”
“Simply, it is the foods that are baked or soaked in soybean oil and ones that are processed for long shelf-life that are creating an extreme imbalance of omega-6 and omega-3 fats in people’s bodies.
Lundell estimates the ratio of imbalance “ranges from 15:1 to as high as 30:1 in favor of omega-6.” A healthy ratio is closer to 3:1”
Dr. Alex Vasquez has also commented on omega-3 fatty acids being a far better choice for reducing the risk of cardiovascular death.
Clean eating and intelligent training should always be the first option before statins are considered.
Here are some other related lifestyle factors you should be aware of:
- Smoking
- Being overweight/obese
- Lack of exercise
- High stress levels and inability to manage emotions
- Pre-existing medical conditions and medications
Regular Blood Work
By no
, you know why insulin resistance and systemic inflammation are the root cause of cardiovascular disease.
Therefore, it is imperative to get regular blood work done so you know exactly what’s going on.
Here is what you should evaluate in the context of inflammation and cholesterol:
- HDL – higher than 70 mg/dL for near zero cardiovascular risk
- LDL – lower than 100 mg/dL
- high-sensitivity CRP (hsCRP) – below 3 mg/dL (indicator of plaque risk)
- Sex hormone binding globulin (SHBG) – between 10-57 nmol/L for men, 18-144 nmol/L for non pregnant females (first indicator of insulin resistance)
- Triglycerides – Lower than 150 mg/dL
You’ll notice I didn’t list total cholesterol here – many high-level doctors have advised me that it is ultimately a worthless test.
The total cholesterol reading takes HDL, LDL and triglycerides all into account.
While total cholesterol levels under 200 mg/DL are typically considered to be good, you are not seeing the entire picture.
You could have a total cholesterol of over 300 and yet have an astronomically high HDL reading.
If a physician put you on a statin in this situation, you would only lower your HDL levels and increase the risk of heart disease.
The same goes for treating high triglyceride levels, as that’s usually a problem with insulin resistance which can be treated with Metformin and extended periods of fasting.
Conclusion: Does Cholesterol REALLY Matter?!

The bottom line is this: High cholesterol is not a “cause” of anything.
It is the END RESULT of hereditary factors and consistently poor lifestyle choices – which are the two primary indicators of problems.
This is why it is imperative to focus primarily on lifestyle changes, as it will fix the real problem and lead to the greatest benefit.
If you want to learn more about how statins are damaging our health, I highly recommend reading this article, which details the cover-up of statin research data.
And while I personally haven’t read this book, A Statin Nation appears to be a worthwhile read.
Sending you lots of love and light!
And as always, don’t forget to join the email list for all the latest updates in the health optimization field.



